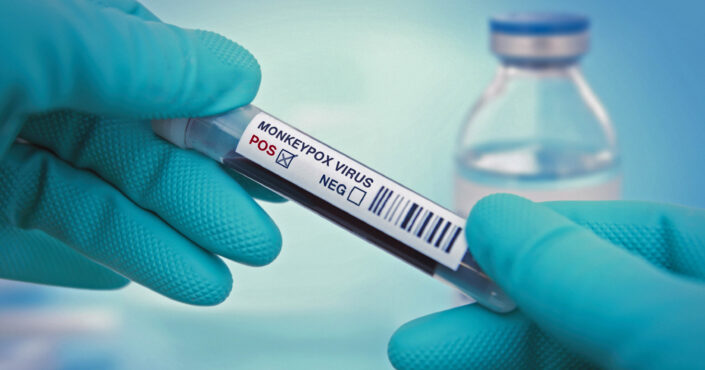
After the COVID-19 pandemic dominated our lives in 2020, 2021 and now 2022, the last thing anyone, especially nurses, wanted to hear about was another pandemic. But here we are again. The Centers for Disease Control and Prevention (CDC) documented the first U.S. case of Monkeypox in the 2022 outbreak on May 18. As of August 24, there were 17,432 cases reported in the United States. There’ve also been over 30,000 cases reported in 89 countries, including 82 countries that never had Monkeypox cases before 2022.
Monkeypox was first identified in 1958 in laboratory monkeys in Denmark, hence the name. However, the first case in humans wasn’t until 1970 in the Democratic Republic of Congo. Before 2022, the virus was primarily contained in Africa, spreading to just 10 countries due to international travel or imported animals. The first 2022 case outside Africa was reported in the United Kingdom in early May, starting the current outbreak.
On July 23, the World Health Organization (WHO) declared Monkeypox an international health emergency. With an increased risk in the U.S., it’s critical for nurses to know as much as they can about the disease.
What Is Monkeypox?
Monkeypox is a viral, zoonotic infection, meaning it originated in animals, and animals likely carry it. It’s similar to smallpox and in the same virus family, orthopoxviruses. There are currently two known strains of the virus, primarily grouped by location. It’s thought that the 2022 outbreak is a new, third strain.
What Are the Symptoms?
When we hear the word smallpox, we get a little nervous. We eradicated it in 1980, but before that, it infected almost 12 million people and killed hundreds of thousands. The first thing every nurse should know about this virus is how to identify it.
During the first five days, a patient will be in the prodromal period, the period after incubation and before the characteristic symptoms of infection occur, which has much more subtle and vague symptoms. These symptoms include:
- Fever
- Intense headache
- Lymphadenopathy (swelling of lymph nodes)
- Back pain
- Myalgia
- Severe fatigue
Unfortunately, these symptoms are also common in infections like COVID-19, the flu and other illnesses, making identification very difficult during this stage.
About four days after the fever starts, the rash appears. This rash is characteristic of the orthopoxvirus family and a more straightforward way to identify the infection than in the prodromal phase. Lesions start as papules, progress to vesicles and finally pustules before scabbing over and falling off after about 14 days. Patients usually describe it as very painful, then itchy as it crusts over.
Lesions are usually present on the:
- Face
- Palms of the hands
- Soles of the feet
- Genitals
They’re peripheral to the center of the body. The number of lesions can range from just a few to 1,000s.
How Is Monkeypox Transmitted?
According to the CDC, animals spread the first cases to humans. The spread was primarily through contact with an infected animal’s body fluids, a bite from an infected animal or the preparation and ingestion of bushmeat (a type of meat common in some regions of Africa that is raw or not processed).
However, in the 2022 outbreak, cases are primarily spread human to human by four different routes:
- Direct contact by touching an infected person’s infected sores, scabs or body fluids.
- Indirect contact through fomites (contact with materials contaminated with infected materials like clothing or linens)
- Respiratory through droplets like covid, but it requires prolonged face-to-face contact to be transmitted (longer than 15 minutes)
- Vertical transmission from a pregnant person to the fetus through the placenta (no cases reported in the U.S. in 2022)
How Is Monkeypox Treated?
Nurses should know and educate patients that most people don’t require treatment when infected. Monkeypox has a low mortality rate, and most people recover without intervention. Treatment primarily focuses on supportive measures and symptom management, such as fever reduction, pain management, etc.
Those who should seek treatment include:
- Patients with severe disease or at risk for severe disease
- Immunocompromised patients (cancer patients, HIV patients, etc.)
- Patients with atypical rash sites, such as the mouth, eyes or genital area
For those who qualify, what is the treatment for Monkeypox? Generally, healthcare providers treat Monkeypox with antivirals, similar to COVID-19. The one used most often is Tecovirimat. This treatment is a 14-day course, with doses based on the patient’s weight.
Cidofovir/brincidofovir has also received approval for treatment, but it presents a high risk for kidney damage. Those with severe rash or when the eyes are affected by the rash may use Triflourodine eye drops and ointments for one to two weeks.
Patients may also receive treatment post-known exposure. When a patient with a known exposure should:
- Get the Monkeypox vaccine ASAP (within 14 days)
- Monitor for symptoms for 21 days
Are There Vaccines?
Yes! These vaccines were developed and used to eradicate smallpox. There are currently two different types of vaccines in the U.S.
1. Modified Vaccinia Ankara (MVA) vaccine
- Brand name JYNNEOS approved for the prevention of smallpox and Monkeypox in the U.S.
- Highly attenuated, nonreplicating vaccine with an excellent safety profile
- Immunocompromised people can use it
- Administered subcutaneously in two doses four weeks apart
The U.S. Food and Drug Administration issued an emergency use authorization (EUA) for the JYNNEOS vaccine, allowing administration of the vaccine via intradermal injection for high-risk individuals aged 18 and older.
2. ACAM2000 vaccine
- Replication-competent smallpox vaccine only allowed for use in select patients due to number of adverse effects
- Approved in the U.S. for the prevention of smallpox
- Can be used for Monkeypox as a CDC expanded access investigational drug due to the global emergency declared by the WHO and the CDC
- Should only be used if the JYNNEOS vaccine isn’t available for high-risk patients
As of August 2022, there’s a minimal supply of the JYNNEOS vaccine in the U.S. While more is expected in the coming months, the exact time frame is unknown.
There’s a slightly larger supply of ACAM2000. But again, this vaccine has a lot of adverse effects and shouldn’t be used in many people, including immunocompromised or pregnant people. Immune response takes 14 days following the second dose of JYNNEOS and four weeks after the ACAM2000 dose. Healthcare providers can use either vaccine to prevent infection following exposure.
Because vaccine supplies are so limited, the only people eligible for the Monkeypox vaccine in the U.S. as of August 2022 include:
- People who have had a sexual partner in the past 14 days who were diagnosed with Monkeypox
- People who attended an event or venue where there was known, close Monkeypox exposure
- Gay, bisexual and any other men who have sex with men, who have had multiple sexual partners within the last 14 days
Monkeypox Isn’t a Sexually Transmitted Disease
In the U.S., 99% of all Monkeypox infections are in men who have sex with men. Since the AIDS pandemic broke out in the 1980s, many stigmas have been placed on the HIV infection itself as a “gay” disease. The same is happening with Monkeypox.
There’s no such thing as a gay disease. Monkeypox isn’t a sexually transmitted illness; viruses can infect anyone regardless of sexual preference or orientation. Anyone can get Monkeypox: men or women; heterosexual, transgender and nonbinary people; and others. Educating our patients on this fact, especially those at risk, helps prevent the stigma from spreading.
Are There Guidelines?
The WHO put out an updated version of its Monkeypox guidelines, primarily focused on testing and tracing, in June 2022. These guidelines include the following:
- Must have a positive PCR test to be qualified as an active test (not just based on symptom report)
- Probable and confirmed cases of Monkeypox should be reported as early as possible, including a minimum dataset of epidemiologically relevant information, to WHO through IHR national focal points
- Healthcare professionals should test people with a rash with no other cause of the rash and present with one or more of the following symptoms:
- Headache
- Fever
- Lymphadenopathy
- Myalgia
- Back pain
- Asthenia (profound weakness)
- Test subjects should also meet one or more of the following criteria:
- Linked to a probable or positive case of Monkeypox within the last 21 days
- Travel history to an endemic country within the last 21 days
- Multiple sexual partners within the last 21 days
- Positive orthopoxvirus vaccine serological assay (in the absence of smallpox vaccine)
- Is hospitalized
- Contact tracing and reporting are essential
As of August 2022, the CDC recommends following WHO guidelines but has its own form of tracing.
How Can Monkeypox Be Prevented?
Another crucial part of education that nurses can give their patients is how to prevent infection. According to the CDC, preventing infection includes the following:
- Avoid close, skin-to-skin contact with people with a rash that looks like Monkeypox
- Don’t touch the rash or scabs of a person with Monkeypox
- Don’t kiss, hug, cuddle or have sex with someone with Monkeypox
- Practice safe sex
- Avoid contact with objects and materials a person with Monkeypox has used
- Don’t share eating utensils or cups with a person with Monkeypox
- Don’t handle or touch clothing, bedding or towels belonging to a person with Monkeypox
- Wash your hands often with soap and water, or use an alcohol-based hand sanitizer, especially before eating or touching your face and after you use the bathroom
- Avoid contact with potentially infected animals found within specific areas of Africa
Are Cases Reported?
In the U.S., medical professionals must report cases to the CDC through one of the following two methods:
- Enter the necessary sCRF (Short Case Report Form) data directly into the CDC DCIPHER platform (found on the CDC website)
- Enter the necessary data directly into an existing jurisdictional case surveillance system configured for Monkeypox reporting, then upload the reporting data to the CDC DCIPHER platform using a CSV file format
If you’re unsure about this, contact your local state public health system, and they’ll walk you through it.
Be Sure You’re Ready
All the information that has come out so far about Monkeypox is reassuring. It has a low mortality rate, it takes a lot longer exposure to spread, and we already have a vaccine that works. However, the last three years have been traumatic for everyone. We’re all scared of another pandemic, whether you’re a nurse or a patient. Because nurses are on the front lines, they can best spread education to their patients. It’s critical to keep yourself up-to-date, so continue to check the CDC and WHO websites for updates.
Remember, your patients are scared and depend on you to provide them with the information, but we’re all in this together.